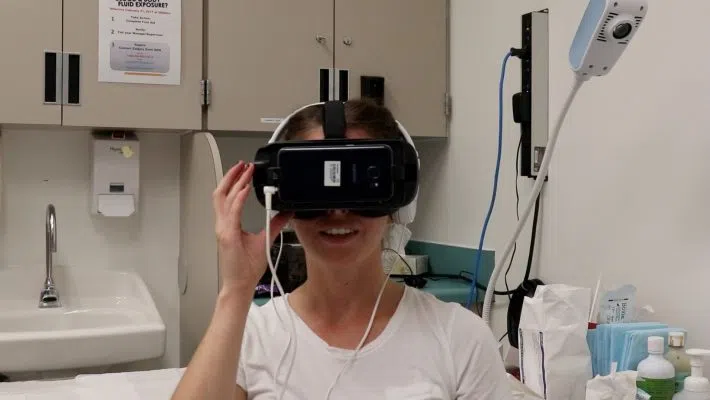
Virtual reality: the futuristic landscape of video games and tech enthusiasts. What role does it play in health care? Could strapping a 350-gram screen just centimeters from your eyes really improve patient outcome?
According to data emerging from Rockyview General Hospital – the first hospital in Canada to use virtual reality – that is an astounding yes.
I met with wound care physiotherapist Jaclyn Frank to discuss this emerging technology and the amazing benefits they are seeing.
“It is so effective, when I look at patient’s pain scores before and after, its amazing how effective it is, our patients love using it and request to have it.”
Frank remarked on the incredible difference virtual reality was making for patients. Normally, coming to the wound care ward meant pain and anxiety, patients would dread the sometimes agonizing experience of having their dressing changed or wounds treated. Now however, this experience is something they can look forward to.
The most dramatic finding coming out of the Rockyview wound care is a 75% reduction in pain and anxiety and a 30% increase to overall patient experience. Those numbers are worth reading twice. Simply distracting the mind and immersing a patient in an alternate reality is able to prevent anxiety and drastically lower pain levels.
But what exactly are they viewing that is keeping them so immersed? Frank said they have 12 different programs loaded on their Samsung Gear VR set that were carefully selected for their levels of distraction, relaxation, and immersion. Some of the most popular calming experiences involved sitting by a campfire and watching the occasional wildlife, sitting on a beach with a guided meditation, or swimming with dolphins underwater. The more intense and immersive experiences included a roller coaster ride or a Cirque Du Soleil show with many performers jumping all over the screen.
I tried the headset myself, and wasn’t too impressed with the cartoonish graphics, though I could not doubt the engagement of the 360-degree view. I swam underwater with dolphins, and felt nauseous on a choppy roller coaster, a symptom not commonly reported by patients.
Video of Swimming with Dolphins Experience.
(Pocket Dolphins, Google Cardboard 2015)
Knowing the technology has already moved passed the programs they were using, I asked Frank if they had any plans to update their virtual reality experiences with better graphics. She told me that a newer system was currently being vetted to ensure it passed all infection prevention standards. Currently, Rockyview has 2 sets of Samsung VR headsets, which were anonymously donated last November. What these two headsets have been able to provide is astonishing. Another anonymous donor had stepped forward eager to donate the Oculus Go, which has better graphics, is more lightweight, and does not require a cellphone to be operational.
When asked why all these donations, Frank had this to say: “I think people are seeing the benefits of it, and are seeing the great work that’s happening with VR and want to help contribute to overall patient experience and say that’s amazing how can I help more patients have this experience”
Graphics will improve, and in many instances animation will be replaced by actual real world photography and videography stitched together which will only deepen patient immersion and distraction to pain. These images are from virtual reality experiences created from composites of many stitched-together panoramic images and will soon render animation obsolete.
- Samsung VR
(Virtual reality images courtesy of Samsung VR, NPR, and NASA)
Rocky View have stated a 30% in patient experience, but what does improving patient experience mean to a patient? I spoke with Graydon Cuthbertson a former patient who the VR system at Rocky View extensively to hear his take. Cuthbertson suffered from the extremely painful Compound Syndrome, and couldn’t speak highly enough of virtual reality stating a “night and day” difference in pain.
Rockyview continues to collect data regarding virtual reality’s influence on the pain and anxiety patients experience. It would follow that more immersive and believable experiences would work even better at distracting patients from painful experiences and the anxiety surrounding them.
Interestingly, Frank told me that It isn’t just the patient having decreased anxiety, it’s also the physiotherapists working in wound care.
“Because our patients are experiencing less anxiety and less pain, we are having less anxiety. We don’t like to hurt people and when we do it, it does cause us moral distress. Its upsetting to have to hurt somebody even though it might be something they need to have done. And when our patients had less anxiety we were finding we felt way better about treating our patients and were able to do a better job at treating our patients.”
Frank said that they were able to do dressing changes a lot more effectively and a lot quicker, since they did not have to stop due to high patient pain levels. This was an effect they didn’t expect to see, but was certainly a pleasant surprise.
These results are causing many health care professionals sit up and take notice. Frank said that they have had a lot of interest since they started this program. Other wards in the hospital such as the Intensive Care Unit (ICU), Coronary Care Unit (CCU), Emergency, as well as Maternity wards are interested in incorporating VR.
Specifically, Rockyview’s ICU/CCU is currently working on a research project right now using virtual reality for relaxation. They are studying its meditative effects and its ability to calm and center a patient, as opposed to the pain control applications the wound care ward is using it for.
While it’s been proven that virtual reality is beneficial in downstream applications like pain management and reduction of anxiety, it has many other benefits that have been and continue to be studied. A significant one is training and education. Specifically, in healthcare, it is being used to simulate surgeries, with one company calling itself “The Flight Simulator for Surgeons.”, as well improving communication skills of medical students, such as how to break bad news to families. And even educate physicians on the experience of being elderly,
Further medical uses include the treatment of phantom limb pain, speeding up recovery from traumatic brain injuries, improving eyesight, improving balance, exposure therapy, and viewing live operations in 360-degrees.
“We are just starting to see the beginning of virtual reality coming into our day to day lives, it’s just going to continue to grow”.
With prices dropping from $1000 dollars to $260 and below, virtual reality is now an accessible reality. Patients can afford to buy and use these systems at home, and hospitals will not have to shell out much money to include these systems in their patient care. Virtual Reality is no longer a gimmicky game, but is now an incredible teaching, rehabilitation, and pain reduction tool with limitless applications. In time, we will see just how much this will transform healthcare.
“The possibilities are endless.”
References and Further Reading:
Simulated Surgery:
https://www.fundamentalsurgery.com/
https://www.fundamentalvr.com/
Empathetic Connection:
https://news.nnlm.gov/ner/2017/06/16/a-new-reality/
http://medicalcyberworlds.com/technology/
https://www.sciencedirect.com/science/article/pii/S0738399116304943
Phantom Limb Pain Link:
https://www.ncbi.nlm.nih.gov/pubmed/28211829
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5825921/
Brain Injuries:
https://www.mindmaze.com/fda-clears-gamified-neurorehabilitation-system/
https://www.medscape.com/viewarticle/897972
Live Operations:
https://www.medicalrealities.com/
Photo Gallery:
http://apps.npr.org/rockymountain-vr/
https://samsungvr.com/view/cM6NfDU2WqU
https://vrscout.com/projects/swimming-with-dolphins-virtual-reality/